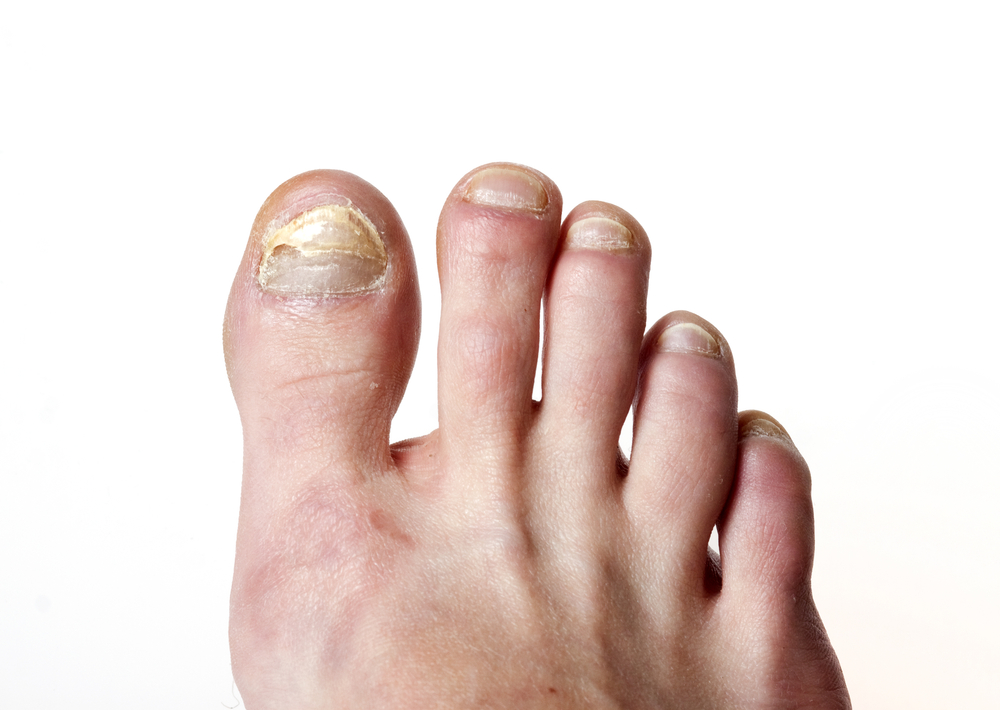
Toenail fungus, or onychomycosis, is a fairly common infection underneath the surface of the toenail that affects about 20% of Americans. Typically, it’s caused by tiny fungal organisms called dermatophytes. (Less commonly, the infection can be caused by molds or yeasts.) Once infected, the toenail often darkens and develops white streaks, becomes thick, and gives off an unpleasant odor. Debris may gather beneath the nail as well.
If left untreated, the infection may spread to other toenails, making it hard to walk. The fungal infection can also travel to your fingernails or skin.